|
These papers prompted discussions on whether MOG-Abs should be considered a marker of a distinct disease entity: this has been confirmed in subsequent studies, based on the abovementioned features, as well as cerebrospinal fluid, imaging, and pathology differences in comparison to AQP4-Ab-seropositive NMOSD and MS 5-7. 
These patients had distinct demographic and clinical features in comparison to those who were AQP4-Ab-seropositive, with less female preponderance, younger age, more frequent involvement of the conus medullaris, greater likelihood of monophasic course and better recovery following attacks in the MOG-Ab group 3, 4. In 2014, two seminal papers described a subset of patients with aquaporin-4 (AQP4)-Ab-seronegative neuromyelitis optica spectrum disorder (NMOSD) who harboured MOG-Abs, detected using the newer assays. 
The significance of these antibodies became clearer in the 2010s, when newer, more specific assays became available that allowed for the detection of the biologically relevant MOG-Abs 2. However, they were also detected in other central nervous system (CNS) conditions such as isolated optic neuritis or myelitis, acute disseminated encephalomyelitis, and cortical encephalitis 1. 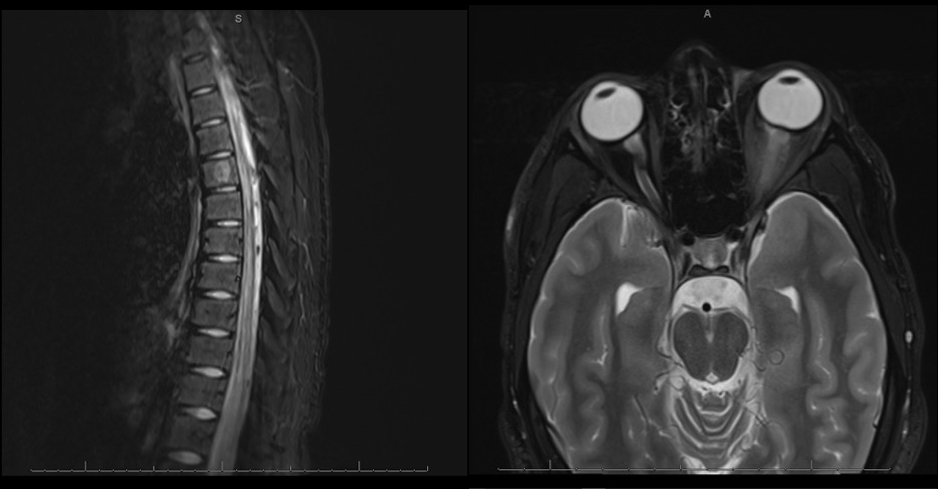
Antibodies against MOG (MOG-Abs) were first identified in patients with multiple sclerosis (MS) in the early 1990s and were then thought to be biomarkers of MS 1. Myelin oligodendrocyte glycoprotein (MOG) is expressed on the surface of myelin sheaths and oligodendrocyte membranes, and is involved in oligodendrocyte microtubule stability, cellular adhesion and the complement cascade 1.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
